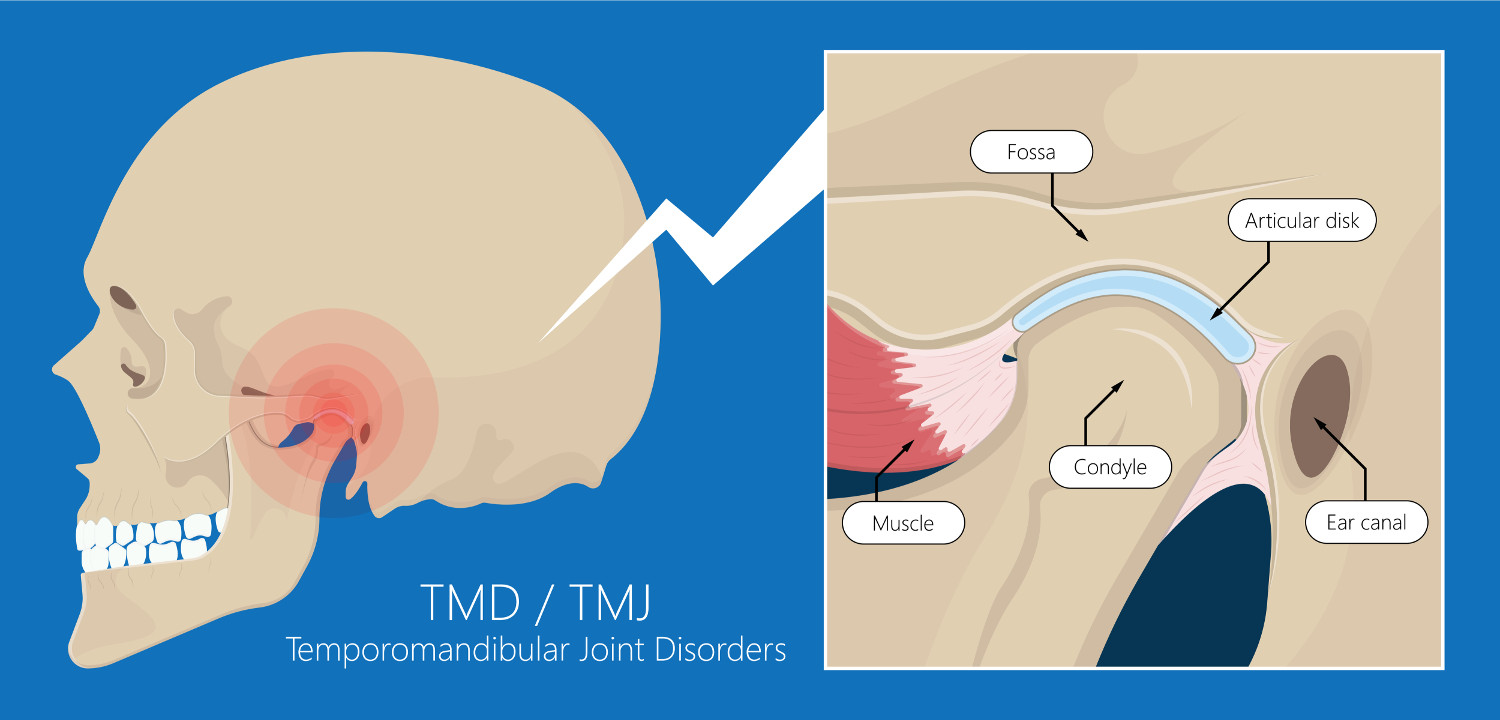
Temporomandibular Joint Dysfunction (TMJ Syndrome)
What is Temporomandibular Joint Dysfunction?
Among patients that regularly visit dental clinics, up to 40% of these individuals may have temporomandibular joint dysfunction 1. Temporomandibular joint dysfunction, also known as TMJ syndrome or TMJ dysfunction, impacts the temporomandibular joint, where the jaw attaches to the side of your skull. Generally, it is an umbrella term covering a broad range of conditions and disorders.
You have two temporomandibular joints on either side of your head. If you place your finger tips on the side of your face in front of your ear and open and close your mouth, you will feel this joint in action. Usually, this joint allows you to talk, chew, yawn, and more - without any pain or disruption. For individuals experiencing temporomandibular joint dysfunction, jaw pain, limited movement, and other symptoms may occur during these activities.
Typically, damage or injury causes temporomandibular joint dysfunction, leading to localized pain in the jaw. Luckily, this condition is usually not very serious and can resolve on its own. In fact, many cases get better without any intervention. Yet, in some cases, treatment may be necessary - as with many individuals that visit dental specialists. In this article, we’ll explore the symptoms, causes, treatment, and more regarding TMJ dysfunction.
What are the Symptoms of Temporomandibular Joint Dysfunction?
What are signs of TMJ Syndrome? How do you know if you have it or not? The common signs and symptoms of this dysfunction or syndrome include the following:
- Jaw pain.
- Pain in the face or neck.
- Jaw stiffness.
- Limited movement of the jaw.
- Popping, grinding, or clicking noises when moving the jaw.
- Locking of the jaw.
- A headache.
- Ear pain.
- Facial swelling.
- Changes in the alignment of the upper or lower teeth due to jaw issues.
- Pain that may get worse when you chew or move your jaw.
TMJ syndrome or dysfunction can also lead to sleep problems due to the pain, which may keep some individuals up at night. It may also get worse during particularly stressful times.
How Long Does Temporomandibular Joint Dysfunction Last?
If your condition is acute, your TMJ dysfunction may last only a few days or a few weeks. For more chronic conditions, the symptoms may come and go, or flare-up over many months. In chronic cases, treatment is often necessary to help improve the condition and decrease pain. However, there are many non-invasive methods to treat the symptoms of TMJ, as outlined below.
Can Temporomandibular Joint Dysfunction Cause Dizziness?
Interestingly, TMJ syndrome can cause dizziness 2. Surprisingly, this condition isn’t limited to just jaw pain. You may experience facial pain or pain on other parts of your head. It can also cause headaches and migraines in some cases. This is likely due to the close proximity of the jaw to the rest of the skull and the tissues that connect here. If any of these structures or tissues come under stress or strain, they may pull on other structures and tissues, leading to further dysfunctions and symptoms.
Can TMJ Cause Burning Mouth Syndrome?
Burning mouth syndrome is a chronic oral condition where burning in the mouth is felt 3. About two-thirds of patients with burning mouth syndrome also have TMJ syndrome or dysfunction 4. Whether or not TMJ can cause burning mouth syndrome is debatable, but it seems the two conditions may be linked.
Can TMJ Cause Thoracic Outlet Syndrome?
Thoracic outlet syndrome is when the space between your collarbone and your first rib narrows. And yes, TMJ disorders may cause thoracic outlet syndrome 5. Experts theorize that this is due to the tightening of the neck muscles, such as the scalenus anterior and the scalenus medius. When these muscles become tight and stiff, they may cause narrowing in the thoracic outlet. In these cases, it’s important that healthcare practitioners identify TMJ dysfunction or syndrome as the cause to help alleviate it.
Is TMJ Syndrome Dangerous?
In the majority of cases, TMJ syndrome is neither dangerous or serious. Many cases resolve on their own. However, in rare instances, it may become so painful that it drastically impacts a person’s life and quality of life. In these cases, it can be considered much more serious and severe. To prevent your TMJ dysfunction from escalating, ensure you seek out treatment early on.
Is TMJ Syndrome Curable?
TMJ syndrome is entirely treatable and curable. As mentioned previously, many cases actually resolve on their own. However, if you experience any jaw discomfort or persistant pain, it’s advised to seek out professional help, such as booking a visit to your doctor or dentist’s office.
What Causes Temporomandibular Joint Dysfunction?
Sometimes, there is no known cause for TMJ dysfunction. In other cases, common causes may include:
Trauma
Trauma to the teeth or jaw can lead to TMJ dysfunction. For instance, clenching or grinding the teeth may lead to pain and problems with the temporomandibular joint. On the other hand, direct blows to the jaw, such as in contact sports or an accident, can dislocate the jaw or cause damage to the cartilage of the joint. TMJ syndrome may also be brought on by recent dental work, especially if the jaw had to be open for lengthy time periods.
Arthritis
Osteoarthritis and rheumatoid arthritis may both impact the jaw joint. In the case of osteoarthritis, the cartilage at the jaw may become worn down through use and time. Rheumatoid arthritis may also occur at the jaw causing inflammation and pain. This type of arthritis is a type of autoimmune disease where the body’s immune cells attack its own tissues.
Bone deformities
These are often formed at birth leading to chronic TMJ issues and pain.
Bad posture
Everything in the body is connected. Bad posture can lead to neck pain which may cause problems with the jaw and surrounding areas.
Stress
Stress is known to cause increased pain, including in the jaw 6. During times of stress, a person prone to TMJ pain may experience flare-ups as well.
In addition, a poor diet or lack of sleep may also lead to TMJ issues. Ideally, you want to maintain a good overall health care routine which would lower your risk of pain and other health issues. Orthodontic braces may also lead to increased jaw pain or TMJ dysfunction, especially right after adjustment. However, this is often an acute condition and the pain associated with orthodontic braces frequently goes away on its own. Lastly, there is some evidence indicating that hormone levels in women may cause TMJ syndrome. However, more research is needed to determine the exact link.
How is Temporomandibular Joint Dysfunction Diagnosed?
There is not one standard test to diagnose temporomandibular joint dysfunction or syndrome, which can make it difficult for health care professionals to make this diagnosis. However, when it comes to diagnosing TMJ issues, most trained professionals use instruments to assess jaw function 7. They also assess and analyze your pain intensity, your psychological distress, jaw function limitations, and more. And when it comes to who diagnoses your TMJ issue, it could be either an ear, throat, or nose specialist or a dentist. Your doctor will refer you to one of these where you will undergo an assessment.
Imaging may also be done to determine what is going on beneath the surface. This may involve x-rays of the jaw, a CT scan to view the joint tissues and bones, or an MRI to examine the structure of the jaw.
How to Treat Temporomandibular Joint Dysfunction
While more research is necessary on TMJ dysfunction, there are various treatment options available, including the following:
1. Resting Your Jaw
While it’s almost impossible to avoid using your jaw entirely, you can take measures to reduce and limit your usage. To avoid aggravating your pain and condition, stick to soft foods that won’t aggravate your jaw. These may include soups or ice cream, and avoiding tough foods, like beef jerky or gum. Limit your jaw movements - this may mean taking it easy for a few days inside watching T.V. or reading, while limiting how much you talk.
2. Reduce the Stress in Your Life
In some instances, TMJ syndrome is brought on by stress 8. As such, it may help to lower the stress in your life through relaxation and breathing techniques. Begin meditating or start planning down time to relax. For some individuals, this can significantly reduce flare-ups and symptoms.
3. Physiotherapy & Exercise
Jaw exercises prescribed by a physiotherapist can help improve function and reduce pain. A physiotherapist may also perform manual therapy to help reduce your symptoms and also restore regular function. Some self-stretching techniques or movements may further help alleviate your symptoms and pain. However, in no circumstances should your exercises cause increased flare-ups or pain. If pain increases, stop performing the exercises - you could be aggravating your condition.
4. Medications
Various medications may help improve symptoms related to temporomandibular dysfunction including:
- Over-the-counter pain medications, such as ibuprofen or acetaminophen.
- Muscle relaxants, such as Soma or Valium. These can help reduce muscle tension, alleviating pain.
- Corticosteroid drugs to help reduce inflammation and swelling.
- And Botox is also occasionally used to relieve tension in the jaw and reduce symptoms.
5. Hot or Cold Therapy
Heat devices or ice can help relieve pain, tension, and discomfort associated with TMJ syndrome. Ice, in particular, can alleviate pain. Whereas, hot devices may help reduce muscle stiffness and muscle tension. Ensure you don’t apply any hot or cold device for longer than 15-20 minutes, while leaving at least 45 minutes in between each application. Further, make sure you place a cloth in between the device and your skin to prevent any damage to the skin.
6. Mouth Guards or Other Mouth Appliances
Also called occlusal appliances, these devices can help individuals reduce their jaw pain. Usually, these devices are soft or firm. However, experts do not know exactly how these devices help. Some theorize that it may prevent movement, allowing inflammation to decrease. It may also prevent causes, such as teeth grinding.
7. Acupuncture
Acupuncture has shown to be an excellent treatment method to reduce jaw pain, specifically for those with myofascial pain 10. Acupuncture works to release endorphins in the site of application. These are your natural pain relievers, and they help alleviate pain, amongst other symptoms. For some individuals, it may take a few sessions to notice a decrease in symptoms. For others, they may notice immediate results. It varies from individual to individual.
8. Surgery
Lastly, surgery for TMJ syndrome is sometimes considered. However, in most cases, surgery is often avoided due to its invasiveness and irreversibility. This is a very rare consideration. Most often, TMJ dysfunction can be treated with non-invasive techniques, like at-home remedies or massage therapy.
Can Massage Help with Temporomandibular Joint Dysfunction (TMJ Syndrome)?
Many small studies have found evidence that massage therapy can help relieve the symptoms associated with TMJ syndrome 11. Massage therapy can contribute to decreased muscular tension and pain, improving your function and condition. However, massage therapy should be part of a holistic treatment plan. Hot or cold therapy can also be used and other recommended treatment options should be followed per your doctor’s or specialist’s advice.
Are you thinking about using massage therapy as part of your TMJ pain management plan? Book an appointment with us today. Depending what is causing your TMJ issues, techniques or methods may vary. At each appointment, we encourage you to communicate with your massage therapist. If anything causes pain or doesn’t feel right, let them know. They will adjust accordingly. You may notice relief immediately or after many sessions. Again, it depends on the severity of your condition and what is causing your TMJ dysfunction in the first place. Massage therapy in combination with other approaches can greatly help reduce pain and muscle stiffness and tension from TMJ syndrome. Discover how massage therapy can help you!
References
1. Alshaban, K., & Waheed, Z.G.A. “Prevalence of TMJ Disorders among the Patients Attending the Dental Clinic of Ajman University of Science and Technology–Fujairah Campus, UAE.” International Journal of Dentistry. 2018.
2. Hodges, J. “Managing temporomandibular joint syndrome.” The Laryngoscope. 1990 Jan;100(1):60-66.
3. Bouckaert, M., Feller, L., et al. “Burning Mouth Syndrome: Aetiopathogenesis and Principles of Management.” Pain Research and Management. 2017 Oct.
4. Munerato, M.C., Tomattis Pineyero Serrano, O.S. “Burning mouth syndrome.” International Journal of Dentistry Research. 2016; 1(1): 14-23.
5. Carai, A., Crotti, F.M., et al. “Post-traumatic thoracic outlet syndrome (TOS).” Acta Neurochir Suppl. 2005;92:13-5.
6. Ahuja V, Ranjan V, Passi D, Jaiswal R. “Study of stress-induced temporomandibular disorders among dental students: An institutional study.” Natl J Maxillofac Surg. 2018 Jul-Dec;9(2):147-154.
7. Schiffman, E., Ohrbach, R., et al. “Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group†.” Journal of oral & facial pain and headache. 2014, 28(1), 6–27.
8. Wright, E.F., & North, S.L. “Management and treatment of temporomandibular disorders: a clinical perspective.” J Man Manip Ther. 2009;17(4):247–254.
9. Warburton, D.E., Nicol, C.W., Bredin, S.S. “Health benefits of physical activity: the evidence.” CMAJ. 2006;174(6):801–809.
10. Wu JY, Zhang C, Xu YP, Yu YY, Peng L, Leng WD, Niu YM, Deng MH. “Acupuncture therapy in the management of the clinical outcomes for temporomandibular disorders: A PRISMA-compliant meta-analysis.” Medicine (Baltimore). 2017 Mar;96(9).
11. Pierson, M.J. “Changes in temporomandibular joint dysfunction symptoms following massage therapy: a case report.” Int J Ther Massage Bodywork. 2011;4(4):37–47.


